Development of student empathy during medical education: changes and the influence of context and training
Article information
Abstract
Purpose
Empathy levels have been observed to often decrease when medical undergraduates move to the clinical years, particularly in the Western countries. However, empathy either remains similar or increases in many Asian medical schools. This study investigated the longitudinal empathy profile of medical students in Singapore.
Methods
Two cohorts of medical students who enrolled in 2013 and 2014 to the National University of Singapore were tracked for 5 years. The Jefferson Scale of Empathy–student version was used. Analyses on the mean of the empathy level and individual factors, year-wise and gender comparison were conducted.
Results
Average response rates for cohort 1 and 2 were 68.1% (n=181–263) and 55.4% (n=81–265), respectively. For both cohorts, there was no significant change across year of study in the mean empathy score. Average scores for both cohorts were 113.94 and 115.66. Though not significant, we observed mean empathy to be lowest at the end of year 5 (112.74) and highest in year 2 (114.72) for cohort 1 while for cohort 2, the lowest level of empathy was observed in year 5 (114.20) and highest in year 4 (118.42). Analysis of subcomponents of empathy only showed a significant difference for cohort one factor 1 (perspective taking) and factor 3 (standing in patients’ shoes) across the study years.
Conclusion
No significant change in empathy score was observed during the transition from pre-clinical to clinical years, unlike many Western and Far-Eastern studies. This might be due to the curriculum and influence of the Asian values.
Introduction
Developing a physician with both the technical and affective skills in medical programs is critical to ensure quality patient care. While the technical knowledge and skills can be learnt through a well-designed curriculum, attributes such as professionalism and empathy are comparatively more challenging to inculcate. Empathy is the ability to understand meaningfully the patient’s situation, perspective, and feelings, as well as to communicate, and to act therapeutically on that understanding effectively with patients’ consent and assistance [1]. Particularly in the context of healthcare today, empathy is viewed as a multidimensional construct that has cognitive, emotional, moral, and behavioral dimensions [2]. It is an important component of the physician-patient relationship and has an impact on clinical outcomes, patient satisfaction, and compliance [3]. Therefore, great importance is placed on developing empathetic physicians.
Besides the impact on patients, empathy also affects the physicians and students. For instance, empathy is linked to their well-being whereby physicians with lower empathy levels are more prone to exhibit symptoms of exhaustion and stress and more likely to be involved in medical malpractice [4]. Likewise, medical students who are more empathetic and show lower burnout tend to have more enjoyment in their life [5].
The change in empathy as students’ progress through their years of study has been well-documented. However, the results are often contradictory. Studies conducted in United States showed a significant reduction in empathy during medical education during both undergraduate and residency training [6,7]. Studies from medical schools in the Far Eastern countries including China, Japan, and Korea have seen an increase in empathy levels [8-10].
A vast number of studies have explored the possible contributing factors behind the change in empathy amongst medical students, be it a decrease or an increase. Traditionally, most research investigated the medical curriculum and educational factors. Having too much content to learn in the packed program and the resulting stress was mentioned as one of the factors for the drop [11]. Conversely, appropriate interventions by the schools such as a medical curriculum that also covers topics such as literature, arts, and sciences with philosophical and ethical classes from the start have been shown to increase empathy [8].
The educational environment also plays a part in that the decline might be due to burnout or depersonalization [12]. In the clinical teaching environment, students are exposed to patients for the bulk of the time and this repeated exposure might have desensitized them and subsequently reduced their empathy. There are also studies focusing on the psychological aspects. For example, Chae et al. [4] in 2007 investigated how calling might have an impact on the relationship between medical school students’ empathy and academic burnout. In general, individuals with a sense of calling are more likely to attach meaning to their work and have higher satisfaction with what they do for a living and are less stressed [13]. The study found that a higher calling and less academic burnout are more likely to result in medical students with greater empathy [4]. Another study involving medical students found that those with a poorer quality of life and more burnout might have lower empathy [14].
In the recent years, researchers have investigated other dimensions of contributing factors. Personal-socio determinants were previously explored where time spent with family, arts, and community service correlated with higher empathy scores, whilst time spent with significant others and individual leisure correlated with lower scores [15]. The authors explained that the interactions with the bigger family allowed more inclusivity and are more nurturing while interactions with one’s significant others or own leisure are more individualistic and exclusive.
Indeed, there are also arguments for Western cultures being known to be more individualistic and Eastern cultures more collectivist [16], with the latter promoting empathy. Ponnamperuma et al. [17] in 2019 conducted a review of cross-sectional and longitudinal studies and found that empathy changes may not be indiscriminate. In fact, there seemed to be a pattern of change influenced by the geo-sociocultural factors. Empathy generally showed small but significant decreases in Western studies and remained relatively constant in the middle regions. Eventually, predominantly small but significant increases in empathy were observed in the far Eastern studies toward the right of the globe [17]. Socio-cultural factors may thus affect empathy levels, for instance, collectivism might increase empathy.
However, medical schools in the South Asian region including the one conducted previously in Singapore, seemed to report no significant change [15]. As this was a cross sectional study where the findings might be affected by baseline differences and variability among the different training contexts that various student cohorts are exposed to, this paper aims to explore how empathy changes longitudinally in the same medical school, and to suggest possible reasons including socio-cultural factors that might play a part. Singapore, located in the “middle region” infused with both the Western and Eastern cultures, provides an ideal situation to possibly explain how socio-cultural factors could contribute to empathy and thus further add to our understanding on the contributing factors of empathy.
Methods
This study employed a longitudinal research design using a quantitative approach and the section below describes the data collection process, sampling of participants, and data analysis. Longitudinal research can be defined as “research emphasizing the study of change and containing at minimum three repeated observations on at least one of the substantive constructs of interest” [18]. Ethical approval was obtained from the Institutional Review Board of National University of Singapore (reference no., 13-143).
The Jefferson Scale of Physician Empathy-Student (JSPE-S) was selected as it has satisfactory psychometric properties [19] and has been validated in a number of different countries, most relevantly in China, Korea, and Japan [8,9]. It has shown good correlation with other measures of empathy [20] and has been also used previously in the cross-sectional study conducted in the school. The JSPE-S is a self- administered, 20-item pen and paper test answered on a 7-point Likert scale. There are both positively and negatively scored questions that are grouped into three factors (factor 1: perspective taking–10 questions; factor 2: compassionate care–8 questions; factor 3: standing in patients’ shoes–2 questions). Before the start of the survey, there are also demographic questions (e.g., name, gender, and age). It offers a quantitative basis of comparison of empathy levels.
Two cohorts of medical students (years 2013 and 2014) who enrolled in Yong Loo Lin School of Medicine, National University of Singapore were invited to participate in the study. The study was conducted starting from year 1 until 2018 and 2019 respectively for the two cohorts whereby they finished their 5-year course. Voluntary sampling was used and hardcopy questionnaire was given to students at the start and end of each academic year, where possible. Data were collected during phase briefings, combined teaching sessions, or exam briefings/debriefs. The investigators briefed the students to remind them the importance of their inputs before each session.
Six data points from each cohort were selected—start of study (year 1), year 2, year 3, year 4, year 5, and end of study (year 5 end). From years 2–5, data from either the end of the study year or start of the next study year were selected depending on student availability and response rate. Item-total score correlations were calculated from the individual item responses on the JSPE-S and analyzed by year of study with one-way analysis of variance with Bonferroni correction. Gender differences of empathy scores were analyzed with two-tailed t-tests.
Finally, after verifying the assumptions of sphericity using Mauchly’s Sphericity test, a repeated measures analysis of variance was performed for the longitudinal study. As respondents were asked to provide their student number, the analysis was done on students who completed all the 6 selected data points to evaluate how their individual level of empathy had evolved over the course of study. Data from both cohorts were combined for analysis for better generalizability. Statistical analysis was done using SPSS ver. 13.0 (SPSS Inc., Chicago, USA).
Results
1. Response
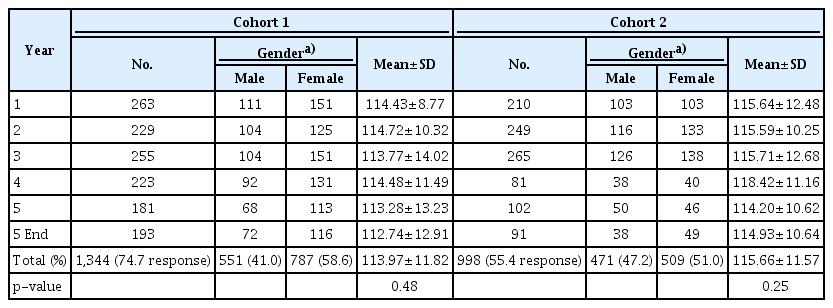
Table 1 shows the descriptive statistics broken down by year of study and gender. A total of 1,344 and 998 responses were received for all 6 data points and the response rate was 74.7% and 55.4% for cohort 1 and 2, respectively. There were more females (58.6%) than males (41.0%) for cohort 1 but genders for cohort 2 were more balanced (47.2% and 51.0%).
2. Mean overall empathy levels
The mean overall empathy level across all the data points was 113.97 (standard deviation [SD]=11.82) and 115.66 (SD=11.57) for cohort 1 (year 2013) and 2 (year 2014), respectively. Cohort 2 had a higher baseline level.
Across the years of study, there were slight differences in the mean empathy level within each cohort. For cohort 1, mean empathy was observed to be lowest at year 5 end (112.74) and highest in year 2 (114.72) (Fig. 1) while for cohort 2, the lowest level of empathy was observed at year 5 (114.20) and highest in year 4 (118.42). Fig. 1 shows how the mean empathy level changes within both cohorts. However, an F-ratio of 0.904 and 1.326, and a p-value of 0.48 and 0.25 for cohort 1 and 2, respectively showed that there was no statistically significant difference in mean empathy levels across the years of study.
In terms of gender, a significant difference in empathy scores was noted between male and female participants (p<0.001) for cohort 1 year 2, but not in cohort 2.
3. Mean for factors
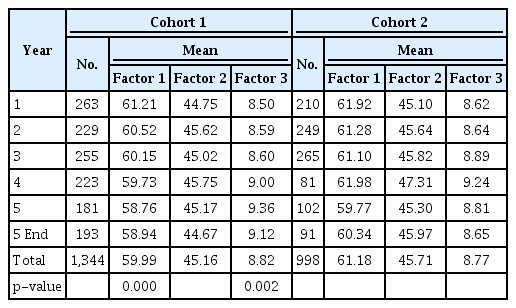
Analysis of the scores for the three factors in the JSPE are shown in Table 2. The overall mean for cohort 1 is 59.99, 45.16, and 8.82 for factor 1, 2, and 3, respectively.
Cohort 1 showed a significant difference for factor 1 and factor 3 when comparing the mean factor levels among the study years within the cohort. The mean score for factor 1 (perspective taking) declined from 61.21 at year 1 to 58.94 at year 5 end. For cohort 1 factor 1, post-hoc analysis revealed that the significant difference was observed when comparing the level between year 1 with that of year 5 and also year 5 end. Factor 3 (standing in patients’ shoes) increased gradually from 8.50 in year 1 to 9.12 in year 5 end with significant difference between year 1 with year 5.
However, for cohort 2, no significant difference was observed for the mean for all 3 factors among the study years. The overall mean for cohort 2 is 61.18, 45.71, and 8.77 for factor 1, 2, and 3, respectively.
Gender wise, significant difference was only observed for cohort 1 year 2 and years 2, 4, and 5 for factor 1 and 2, respectively.
4. Individual student tracking
For the tracking of individual student’s empathy, data from a total of 31 students were analyzed. There was a violation of sphericity (p=0.000) and Epsilon Greenhouse Geisser was less than 0.75. Hence, p for Greenhouse-Geisser was taken and the value (0.185) showed that there was no significant difference for the empathy levels of the students across years.
Discussion
We examine the findings and possible explanations including the socio-cultural aspects from various angles such as inherent cultural values and educational interventions.
The mean overall empathy values were 113.97 and 115.66 and ranged from 112.74 to 118.42 for both cohorts. When comparing the single mean value of 114.69 in this study with other longitudinal studies, the value is generally higher than schools in Far Eastern countries like South Korea (109.10, from a university with both the Medical College and Medical School courses) [21] but slightly lower than Western countries such as United States (115.50, from three medical schools in Chicago) (approximate values derived from graphs) [22]. This might be due to various factors.
First, from a socio-historic aspect, the nation was founded by the British in 1819 and was under its governance for more than a hundred years. The medical school started in 1905 and had its medical curriculum shaped after the British system since its inception [23]. Also, despite being an Asian country predominantly made up of immigrants from China, Malaysia, India, and other Asian countries, English has been the language of instruction with mandatory training in one’s mother tongue being a requirement in the local school system. This confluence of Asian and Western cultures may have impacted the empathy scores resulting in mean scores that hovers between that of most medical schools in the West and East [15].
Deep-rooted heritage and cultural values, evolving social factors in Singapore could have also influenced the culture and empathy levels of the students. Being an open economy with good access to internet, many young individuals regularly use their digital devices and often browse the internet and the social media. This increased access to social media and information from various countries in both the Western and Eastern cultures might have an impact on the students’ thinking and lifestyle [24]. Youngsters here also like to watch dramas such as Korean and American shows from sources such as Netflix. Similarly, some medical students reside on campus and interact with international exchange students. Therefore, they are exposed to the cultures and traits from both sides and might have been subconsciously influenced resulting in their empathy level lying between that of the East and West students.
Unlike many Western and Eastern studies which reported changes in empathy as students’ progress in their studies, our findings did not find any significant changes in students’ empathy. While there was a slight decrease in the total empathy score during the transition from pre-clinical to clinical years, this was non-significant and contradicts the Western literature, where the level often significantly dropped when students moved to the clinical years. Western cultures are known to be more individualistic and Eastern cultures more collectivist [25]. Individualism is more common in societies where the ties between individuals are not as close, where people often tend to look after themselves and their immediate families. Conversely, collectivism pertains to places where people are integrated into cohesive in-groups, which throughout people’s lifetimes continue to protect them in exchange for unquestioning loyalty [16]. As collectivism promotes emotional behavior towards others, this may be a reason why the majority of Far Eastern studies showed a positive empathy change while vice-versa was true for the individualistic cultures seen in the West. As such, it is not surprising that Singapore, with a mixture of Western individualism and Eastern collectivism, reported no key change.
Apart from the socio-cultural factors shared above, educational interventions by the school especially during the clinical years might have helped to increase or sustain the empathy levels. The initial findings from the previous cross-sectional study have helped the school in enhancing some of the existing programs. Interventions were introduced early and throughout the course of study. Key initiatives are discussed below.
For students, one of the changes is “the longitudinal patient experience program” where year 1 students from medical, nursing, and pharmacy programs work with families of patients with chronic illness. Students are encouraged to better understand the viewpoints of the patients and their family and more emphasis is given on the importance of sustaining empathy. By expanding their viewpoints to other groups, this might have contributed to the increase in factor 3 (standing in patients’ shoes).
“The patient-based program” is also introduced to year 1 students, with one of the learning outcomes being to establish rapport and determine concerns and feelings of patients using the Master Interview Rating Scale as the key communications teaching tool, which has an empathy component. Next, the value of being empathetic is repeated during the communication skills training program for year 2 students. By exposing students to patient contact early in the curriculum to experience their viewpoint, this could help in the development of empathy by allowing them to reflect on their behavior, actions and experiences with patients [26,27].
We observed that there was an increase in empathy during year 4 for both cohorts; however, this was not significant. A review of the curriculum revealed that this could be due to the postings in year 4 where the students do clerkships in specialties such as psychological medicine, geriatrics, rehabilitation, special care where they interact with patients in need of support. Additionally, the postings are more community-based rather than institutional, exposing students to the broader spectrum of people. These postings come at the time where empathy is expected to drop. Being Asians who are generally more hierarchical and respectful where one is often expected to show filial piety or respect for one’s parents and elders [28], some of these postings could have invoked the empathy nature in them when they deal with the elderly for instance.
The student assessments during these phases also include their professionalism, communication, and teamskills and direct feedback to them is given through workplace-based assessment tools. Such feedback both formative and summative is known to drive student learning and change their behaviors [29]. The repeated assessment of the students’ empathic abilities in their curriculum could have instilled in them the importance of this trait, more so in Singapore where competition in schools is extremely high.
There are several limitations and challenges to the study. First, a key challenge was finding an appropriate time for data collection and obtaining high response rates. The medical program timetable is extremely packed and clinical students are usually divided into groups at various clinical training sites or elective. Although we worked closely with the curriculum team to identify appropriate sessions to administer the questionnaire, we could not administer it at the same month of the year.
Next, there might be certain biases of respondents since this was a voluntary study and those who responded could have been more empathetic or interested about empathy. Also, there might be questionnaire fatigue as students had to fill the form many times, albeit over a regular interval. The research team tried to alleviate this by getting the medical students who helped with the project to encourage their peers to participate. For tracking, the findings may not be representative of the entire cohort as the sample size was too small. The gender difference observed in cohort 1 could be due to the fact that there were much more females than males amongst the respondents.
Finally, we should note that socio-cultural factors may be subjective and differ from individual to individual even in the same country. Further studies such as qualitative interviews could be conducted to get more insights into the cultural factors from the students’ perspective as well as how some of the educational interventions could have sustained their empathy.
In conclusion, the occupancy of a middle ground in relation to the Western and Eastern countries is not surprising when viewed from socio-historic and socio-cultural perspectives as discussed above. Schools can consider planning interventions aligned with the cultural values, as culture can shape an individual’s empathy level, especially when the interventions are appropriate and timely. While these findings are only based on one medical school, we hope that it allows a deeper understanding on how socio-cultural factors may play a part in shaping empathy.
Acknowledgements
We would like to express our gratitude to Dr Gerald Sng, Dr Joshua Tung, and Dr Daniel Tung for their involvement and contributions to this study when they were students at the school. We would also like to thank the Asia Pacific Medical Education Network (APME-Net) members for their inputs when this study was presented at the Niigata Meeting.
Notes
Funding
This study was supported by the Teaching Enhancement Grant from the Centre for Development of Teaching and Learning, National University of Singapore.
Conflicts of interest
No potential conflict of interest relevant to this article was reported.
Author contributions
All the authors contributed to the following roles: conception or design of the work, data collection, data analysis and interpretation, drafting the article, critical revision of the article, and final approval of the version to be published.